Dental implants don't fail overnight. They fail gradually — through peri-implantitis that goes undetected, bite loads that exceed what the prosthesis was designed to handle, or oral hygiene routines that are almost right but not quite. The surgery is the beginning of a long-term relationship between your implants and how you maintain them. This guide covers what that maintenance actually involves, why each element matters, and what to watch for.
The First Six Weeks: The Critical Healing Window
Osseointegration — the process by which bone grows around and bonds to the implant surface — is most active in the first 6–8 weeks after surgery. During this period, the implants are most vulnerable to the micromotion that disrupts integration. This is why the soft diet restriction during this phase isn't optional advice. It's a clinical requirement.
Immediately after surgery: rest, ice packs to the cheek in 20-minute intervals for the first 24 hours, and prescribed medication taken on schedule. Sleep with your head slightly elevated for the first few nights to reduce swelling. Avoid strenuous physical activity for the first 72 hours. No smoking — smoking significantly reduces blood oxygen levels in the healing tissue and is the single most modifiable risk factor for early implant failure.
Oral hygiene starts gently from day two. Saline rinses (half a teaspoon of salt in warm water) after meals keep the surgical sites clean without disrupting blood clot formation. Brushing around the provisional prosthesis with a soft-bristled brush begins once initial tenderness reduces, typically day three to five.
Daily Oral Hygiene: What the Routine Actually Looks Like
All-on-4 and All-on-6 prostheses create a unique hygiene environment. The bridge sits just above the gum tissue, and the zone between the gum and the underside of the prosthesis — called the pontic area — is where plaque and bacteria accumulate if not actively cleaned.
Brush twice daily with a soft-bristled toothbrush or electric brush, working around the gum margins and the surfaces of the prosthesis. Non-abrasive fluoride toothpaste. This alone is insufficient for the pontic area.
Water flosser (oral irrigator) daily — this is non-negotiable for implant bridge patients. A water flosser at medium pressure directed under the bridge and around each implant abutment clears debris and disrupts bacterial biofilm in areas a toothbrush physically cannot reach. This is the single most important addition to a standard brushing routine for All-on-4 and implant bridge patients.
Interdental brushes at the pontic margins where the prosthesis meets the gum. These small brushes reach under the bridge and around implant connections more precisely than floss.
Antibacterial mouthwash twice daily in the first few months, and periodically thereafter — particularly after any signs of gum tenderness or when systemic illness is present.
Professional Maintenance: The Schedule and What It Involves
Home hygiene maintains between appointments. Professional cleaning is what removes calculus (tartar) deposits that cannot be removed by brushing and flossing alone and that, if left, create conditions for peri-implantitis.
During the integration period: professional cleaning every 8–10 weeks, with radiographic assessment at the 3-month appointment to confirm osseointegration. After final prosthesis delivery: biannual professional maintenance appointments minimum. These include cleaning of the prosthesis surfaces and around the implant margins with instruments that are safe for titanium surfaces (not standard steel scalers, which can scratch implant surfaces and accelerate biofilm accumulation).
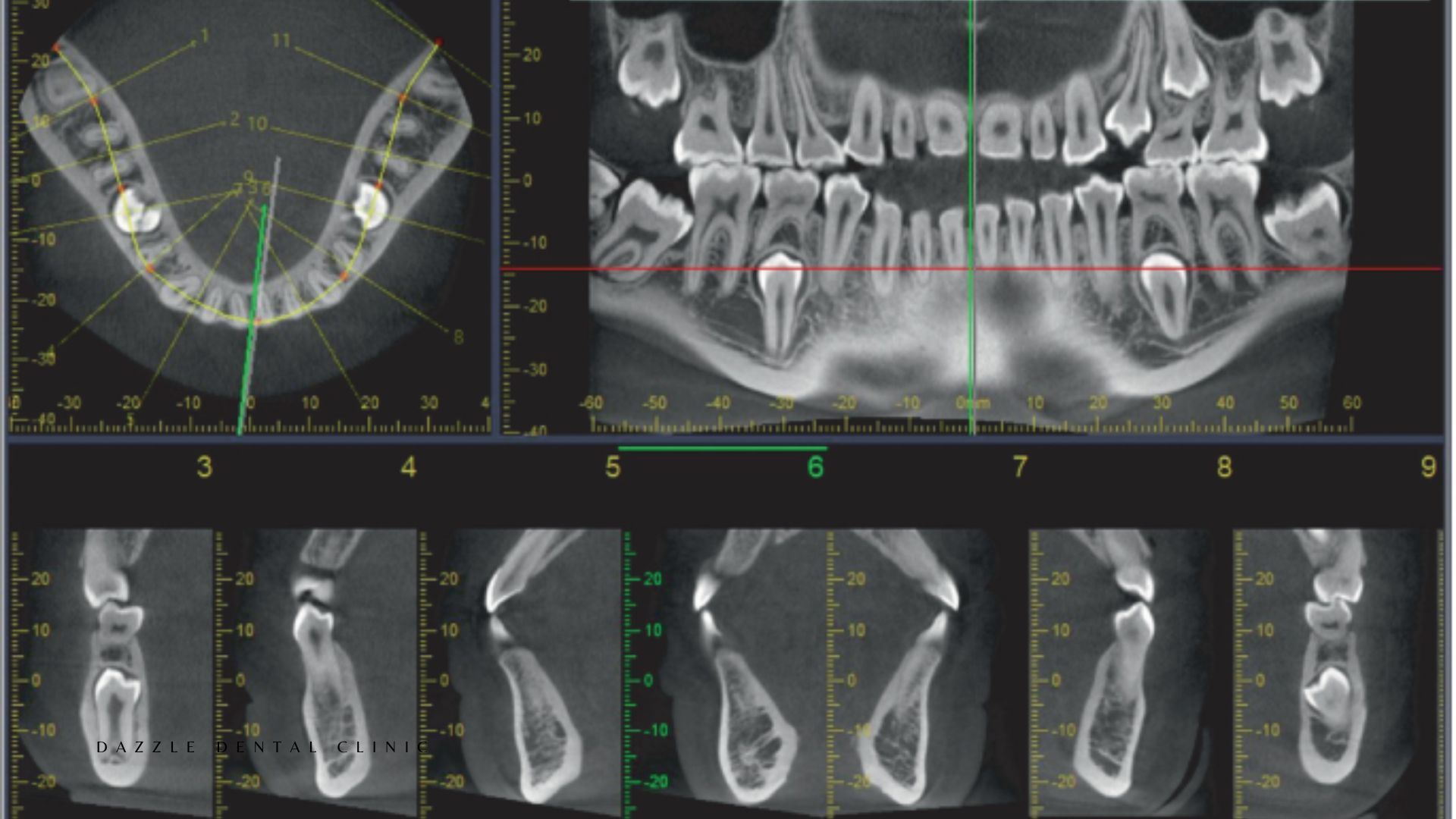
Radiographic monitoring — periapical X-rays around each implant — annually in the first two years, then every two to three years if stable. Marginal bone levels are measured to detect early resorption before it becomes clinically significant.
Managing Bite Load: Nightguards and Bite Checks
The prosthesis and implants are designed to handle normal functional load. Parafunctional load — grinding (bruxism) and clenching during sleep — is not normal functional load. Bruxists can generate bite forces 6–10 times higher than normal chewing. Over time, this fractures prosthesis components, damages implant connections, and can cause marginal bone loss.
If you grind your teeth, a custom nightguard is not optional — it is the most cost-effective way to protect a significant investment. The nightguard absorbs and distributes peak forces that would otherwise be transmitted to the prosthesis and implants while you sleep. Patients are often resistant to wearing one; we encourage you to think of it as maintenance for a restoration that cost a significant sum to place.
Periodic bite checks — at each maintenance appointment — ensure the prosthesis is distributing load evenly across all implants. Uneven occlusal contact creates concentration points of higher stress. Small adjustments made early prevent larger complications later. See our article on occlusal load management in implant success for the clinical detail behind this.
Early Warning Signs to Act On Immediately
Peri-implantitis — bacterial infection around the implant — is the leading cause of late implant failure. It is largely preventable with good hygiene but can develop even in diligent patients, particularly around implants in unfavourable positions or in patients with a history of periodontal disease.
Contact us promptly if you notice: bleeding around the implant margins that doesn't resolve; persistent bad taste or odour from around the bridge; visible gum recession around an implant; mobility of the prosthesis; or pain on biting that wasn't present before. Early-stage peri-implantitis is treatable. Late-stage peri-implantitis with significant bone loss around the implant is much harder to resolve.
For International Patients: Maintenance Coordination
Patients who had their implants placed at Dazzle and have returned home can maintain their implants with their local dentist — we provide a detailed post-treatment report and maintenance protocol. Radiographs taken locally can be shared with our team for remote review. If you notice any of the warning signs above, contact us directly; we can advise whether a return visit is warranted or whether local treatment is appropriate.
FAQs
Q1: How often do I need professional cleaning for my All-on-4 implants?
Minimum twice a year. During the first year, every 3–4 months is recommended to monitor osseointegration and catch any early soft tissue changes. After the first year, biannual maintenance with annual radiographic review is the standard protocol at Dazzle.
Q2: Can I use a regular toothbrush and toothpaste?
Yes to a soft-bristled brush. Avoid abrasive toothpastes (whitening pastes, baking soda formulas) on zirconia or acrylic prostheses as they scratch the surface, increasing plaque retention over time. Non-abrasive fluoride toothpaste is appropriate.
Q3: What happens if I don't wear my nightguard?
For patients who grind, not wearing a nightguard dramatically increases the risk of prosthesis component fracture over time. It also increases marginal bone stress around the implants. Many prosthesis repairs that patients present with are directly attributable to unprotected bruxism. The nightguard is a small recurring investment relative to what it protects.
Q4: My gums look a little red around one implant. Should I be worried?
Localised redness or bleeding around an implant margin should be assessed, not monitored at home. It may be nothing more than local irritation from food impaction or suboptimal hygiene in that area. It can also be early peri-implantitis. Getting it checked within 1–2 weeks is the appropriate response — not waiting to see if it resolves.

















.webp)


.jpg)






