Most wisdom tooth anxiety comes from not knowing what the procedure actually involves. Patients imagine something dramatic. The reality — for the vast majority of cases, including impacted teeth — is considerably more manageable than expected. What actually determines comfort and outcome is the surgeon's skill, the quality of anaesthesia, and how well you follow post-operative instructions.
Here's a clear, honest account of what wisdom tooth extraction at Dazzle Dental Clinic involves, from diagnosis to recovery.
Do Your Wisdom Teeth Actually Need to Come Out?
Not every wisdom tooth needs extraction. The decision is based on clinical and radiographic assessment. Extraction is typically recommended when a wisdom tooth is impacted (stuck in the jaw, unable to fully emerge), causing crowding or displacement of adjacent teeth, is partially erupted and repeatedly infected (pericoronitis), has developed an associated cyst, or is decayed in a position that makes it impossible to treat conservatively.
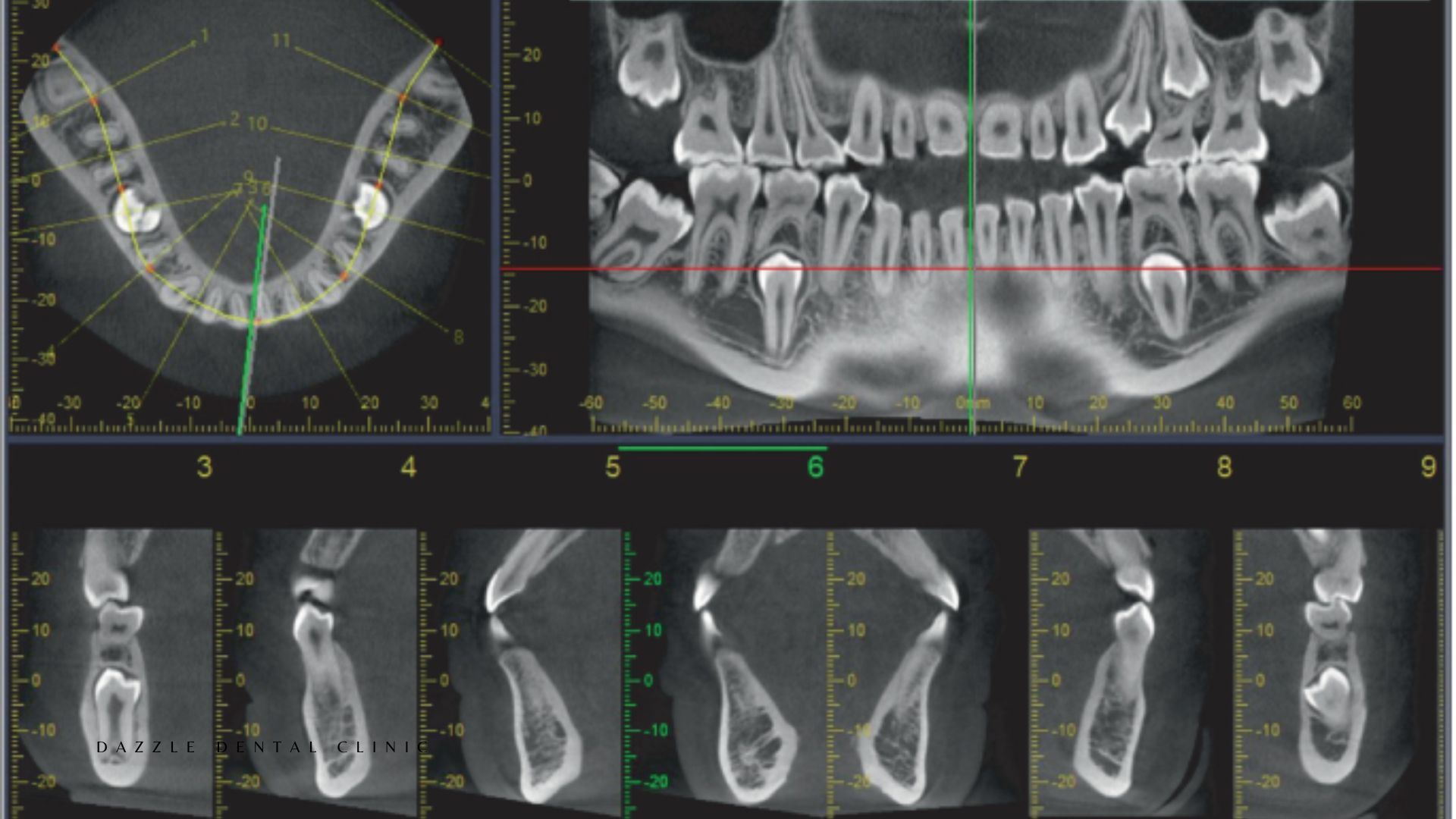
Some fully erupted wisdom teeth that are healthy and functioning correctly can be left alone. We won't recommend extraction unless there's a sound clinical reason. Our assessment includes digital X-rays and, for complex cases, a CBCT 3D scan to map the tooth's exact position relative to the inferior alveolar nerve — a critical safety step for lower molar extractions.
The Extraction Procedure: What Actually Happens
Simple extraction applies when the wisdom tooth is fully erupted, accessible, and has straightforward roots. Local anaesthesia is administered, the tooth is elevated and removed, and the socket is dressed and closed. The procedure typically takes 15–30 minutes. Patients consistently report that the anticipation was worse than the experience.
Surgical extraction is required for impacted teeth — those that are lying horizontally, partially buried in bone, or positioned in proximity to the nerve canal. Our specialist oral and maxillofacial surgeon makes a minimal incision in the gum, removes a small amount of bone to access the tooth, sections the tooth if necessary to minimise the amount of bone removal, and extracts it in pieces. The site is sutured and dressed. Surgical cases take 30–60 minutes depending on complexity.
Throughout either procedure, patients should feel pressure and movement — not pain. If discomfort is felt at any point, additional anaesthesia is administered immediately. We don't proceed through discomfort.
For patients with significant dental anxiety, sedation options including IV sedation or general anaesthesia are available — allowing the extraction to be completed while you are relaxed or asleep.
Recovery: The Realistic Timeline
First 24 hours: Some bleeding from the socket is normal — firm pressure with gauze for 30–45 minutes controls this in most cases. Avoid rinsing, spitting forcefully, or using a straw, as these actions can dislodge the blood clot that's protecting the socket. Cold packs on the cheek in 20-minute intervals reduce swelling.
Days 2–4: Swelling typically peaks at 48 hours and then begins to reduce. Pain during this period is usually managed comfortably with the prescribed medications. Soft foods — soups, yoghurt, scrambled eggs — are recommended. Avoid smoking entirely during the healing period; it's the leading cause of dry socket, a painful complication.
Days 5–7: Sutures (if placed) are reviewed and removed at this appointment. Most patients are comfortable returning to normal diet and activities by day 5–7 for simple extractions; surgical cases may take 7–10 days for full comfort.
What to watch for: Dry socket (a throbbing, deep ache starting around day 3–4 that doesn't respond to standard pain relief) requires prompt attention — contact us immediately. Signs of infection (worsening pain after day 4, swelling spreading, fever) also warrant early review.
Why Surgical Expertise Matters for Impacted Teeth
Lower wisdom teeth frequently lie close to the inferior alveolar nerve, which runs through the lower jaw. Careless extraction technique risks temporary or, rarely, permanent altered sensation in the lip and chin. Our maxillofacial surgeon uses CBCT-guided planning and precise sectioning technique to minimise nerve proximity risk. This is why the surgeon performing the procedure — and their specific training in third molar surgery — matters for complex impaction cases.
What About International Patients?
Some of our international patients from the UK, GCC, and Australia schedule wisdom tooth surgery during planned visits to Mumbai, particularly for impacted cases where the waiting list at home is long or cost is a concern. We can provide radiographic assessments remotely and schedule surgery during your visit. Recovery is well underway within a week, fitting within most travel windows.
FAQs
Q1: How painful is wisdom tooth extraction?
The procedure is performed under local anaesthesia — you'll feel pressure and movement but not pain. Post-operative discomfort is typically manageable with prescribed pain relief and peaks at 48 hours. Most patients describe the experience as significantly less severe than they anticipated.
Q2: How long does recovery take?
Simple extractions: most patients are comfortable within 3–5 days. Surgical extractions of deeply impacted teeth: 7–10 days for meaningful comfort, 2–3 weeks for full tissue healing. Individual recovery varies based on case complexity and how closely post-operative instructions are followed.
Q3: Can I eat before my extraction appointment?
For procedures under local anaesthesia only, eating beforehand is fine. If you're having IV sedation or general anaesthesia, fasting guidelines apply — we'll provide specific instructions at booking.
Q4: Is it dangerous to leave an impacted wisdom tooth untreated?
Partially erupted impacted teeth carry ongoing risk of pericoronitis (recurrent infection), which can become serious. Deeply impacted teeth can develop cysts over time that damage adjacent teeth and bone. Asymptomatic, fully impacted teeth with no pathology may be monitored rather than removed — but this requires a clinical decision, not a waiting approach based on absence of symptoms.

















.webp)


.jpg)






